In case you missed part 1, read part 1 first before continuing.
I sat down in the cold exam room, went to my happy place like I always do, imagining I’m walking on a beach at sunset, and waited for the assistant to tell me my blood pressure looked great and send me home.
140/87
Crap! My heart sunk and I dropped my head on the table. I was literally in shock. I had felt SO good after last night’s visit and talking with the midwife. I didn’t even think I needed someone at the appointment this morning and I had plans for the day. What did this mean?!
She couldn’t tell me anything and said the midwife I was seeing would be in soon. A few minutes later I hear Janelle (the same midwife I saw earlier in the week) talking about calling the hospital for induction outside my door. A few minutes later she opens the door and said it’s time.
I got Justin on speaker phone quickly and she started talking. Janelle explained we couldn’t wait any longer and even though it’s just right at the 140/90 mark that they take gestational hypertension very seriously and they needed to induce me today, tomorrow at the latest.
Knowing my history of a very fast labor with my first and that I had an unmedicated birth center birth, she knew this was the furthest from what I wanted.
Quick recap from birth #1: 3-5ish hours of back labor at home while Justin slept, arrived at the birth center at 10 cm and baby was out in 3 pushes. Read the whole birth story here.
I imagined being stuck in a hospital, tied to a bed by an IV pole and monitors, and nurses just drugging me forcing my body to have a baby when it wasn’t actually ready yet.
The thought of induction terrified me!
And now it was happening. This was turning in to reality.
She said head home, get your husband, pack the last minute things, say goodbye to the toddler, and get back to the hospital to be induced that afternoon.
She checked me before sending us to the hospital to see if I had made any progress since I had been checked a week and a half ago. Major TMI but as she was checking to see how far dilated I was she just started laughing and said my cervix was so soft it was literally just flopping around and she was having a hard time getting a finger in to see how far dilated I was. At least that was a good sign and gave me hope that my body might be able to do this thing even though I was still only at 1cm.
Our last picture as a family of three and so ready to fill that crib with a squishy newborn.

When we arrived at the hospital for the third time that week I knew it was going to be different when we got to the desk and they had all our information filled out and sent us to a room right away, rather than triage. This was it. There was no going back now. We were not going to be walking out those doors again without our baby girl in our arms.

After what seemed like hours of answering preliminary questions and being poked and prodded — apparently I’m a really hard poke and I still have the bruises to prove it two weeks later — they finally brought me the first dose of misoprostol at 4:20pm Friday night.
Misoprostol is used to soften the cervix or induce contractions to begin labor.
The goal was to give me a few doses of misoprostol every 4 hours and see how my body reacted. Since my first birth went really fast and smoothly, they were hoping my body would just kick into gear and I wouldn’t have to be fully induced with intense drugs.
With my first pregnancy we did Bradley Method birth classes and I was also super involved with a local doula class that talked a lot about asking about options and questioning doctors throughout the process. Not that I didn’t trust them, but I wanted to be fully informed the whole way. I’m so glad I had gone through those classes and felt comfortable questioning the medical staff. For example, they wanted to start IV fluids when I first admitted and I requested to drink more fluids to avoid the added fluids. I know my body is powerful and is made to grow and birth a baby. I am so grateful for western medicine but I also wanted to feel comfortable with every decision that was made while we were in the hospital.
On Friday night we mentioned to the midwife who was on duty about our birth plan. Granted, things had changed since we were no longer going all-natural but induction instead, however, she was so open to everything written and sat for 10-15 minutes reading over our birth plan and discussing what we preferred. She also said she would put a copy at the front of my chart and that all the nurses would read it who helped with my care.
One thing important to me was I did not want to be asked about the pain scale. Nurses are notoriously known to always ask about your level of pain, but as I learned in the doula class I attended with my first, being asked to rate your pain makes you think more about how much pain you’re in. Instead I asked that they just ask how am I feeling and allow me to guide the conversation throughout labor. I also requested that no one mention pain medications or ask me about them unless I brought it up. That request turned crucial as labor progressed and things got more intense the next day. I’m so glad I had all my wishes written down and that our birth team was attentive to my desires.
The midwife on duty that night suggested rest as much as possible, sitting on the fitness ball, or sitting cross legged in bed to encourage baby to move down and let the drugs do the rest of the work. The goal was for me to save up energy for when things got more intense.
My sister ended up coming to the hospital and hanging out with us while we watched the Gilmore Girls revival. I also decided it would be a good time to finish some last minute things for work until they came to check my blood pressure and it was the highest it had ever been. Our nurse came back a few minutes after the high bp reading with orders from my midwife to put my computer away and no working until after the baby was born.

At 8pm I got the second dose of miso and the third dose around midnight. It was a rough night attempting to sleep in an uncomfortable labor & delivery bed that is designed to come apart for birth. Thankfully, the husband got some sleep on the couch in our room.

By the third dose at midnight I was feeling much more consistent period like cramping but nothing too significant. Around 1:45 I woke up to my nurse hooking up a bag of IV fluids as she explained to me my contractions were too close together and they needed to get them further apart to be more productive so that my cervix would have time to soften and give baby time to move down. She was still pretty high when I was checked upon admission.
This was my conversation with my sister around 1 in the morning. You can see on that bottom picture how close together and consistent contractions were. It was fun to watch that monitor and see what was going on since apparently I have a high pain tolerance and didn’t realize that was the real gig.
I was supposed to get another dose of miso at 4am but the midwife on call was trying to decide if my body was kicking into gear on its own or if it needed another boost. She checked me to see how progress was going and I was only at about 1.5cm and the baby was still at -3 meaning she still had quite a bit to move down. She decided it would be a good idea to wait and see how the rest of the night went and give my body time to either slow down or pick up more with the intensity.
At 7am the nurses switched and it was my favorite nurse who we had the night before, Amanda. I was so happy to see her!! She told me to order breakfast quickly because that would probably be the last thing I ate before baby was born since they were most likely going to be more aggressive in the coming hours to get baby out.
Around 7:30, our birth photographer and dear friend, Nakalan, arrived to hang out until baby was born. It was so great to have her hang out with us. She barely made it to Clara’s birth since things went so fast and we had been texting on and off all night trying to decide when she should come up.
P.S. Local friends, if you need family photos taken, definitely check her out! She’s amazing and does all of our photos. You can see gender reveal photos here, Clara’s birth photos, 6 month family photos, and pregnancy announcement photos.

Around 8:30am Molly came in, the same midwife who had checked me in the day before and I’d seen one other time at our doctor’s office. We talked about what our options were and what the plan was to get baby out that day.
At that point I was still having consistent “contractions” every 1.5-2 minutes that lasted about 30 seconds. They didn’t really hurt though and was still just uncomfortable back pain.
Molly suggested changing things up rather than another dose of miso. The plan was to insert a foley balloon to get me to 3cm and then start Pitocin, however, when she checked me I was already at 3cm so the foley balloon would just fall out if placed. That was the best news we had all night!!
While she was up there she asked about stripping my membranes. I said go for it!
If you’ve ever had that done you know how uncomfortable it can be. I just laid on the bed laughing as she swept her hand back and forth and said “well you’re 4cm now!” Haha. All that action up there and she was able to get me another centimeter dilated. I’ll take it!
At 8:45 they started a Pitocin drip at 2ml and said they can bump it up every 30 minutes. Almost immediately I started feeling more consistent contractions but nothing too bad and Molly said whatever you do try and stay out of bed and keep moving or sitting upright. We decided to start walking the halls. My little sister came and brought coffee for Justin and they took turns pushing the IV pole with pitocin, fluids, and the monitors.
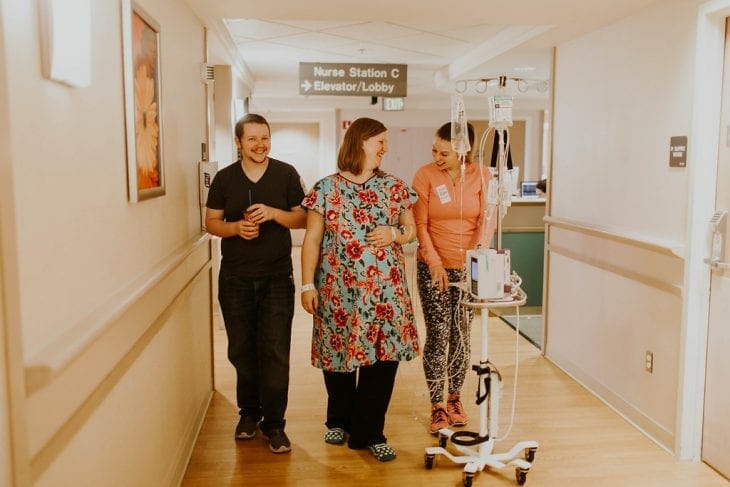
We walked back and forth in the hallway for about an hour until my midwife, Molly, motioned us back to my room. She had been watching my contractions and wanted to break my water if I was okay with that. I knew once the water was broke that meant baby needed to come out within about 12 hours or the risk of infection increases tremendously.
I was so ready to meet our baby girl!
At 11:45am, she pulled out the long crochet hook looking thing and said there would be a pop and a gush. I shut my eyes imagining what it would be like and not wanting to miss out on the birth experience this time around.
One little jab with the hook and it felt like I had just been submerged in a hot tub. No pain and no pop. Such a weird feeling.
At that point I moved to the fitness ball to encourage baby to move down and hang out there.
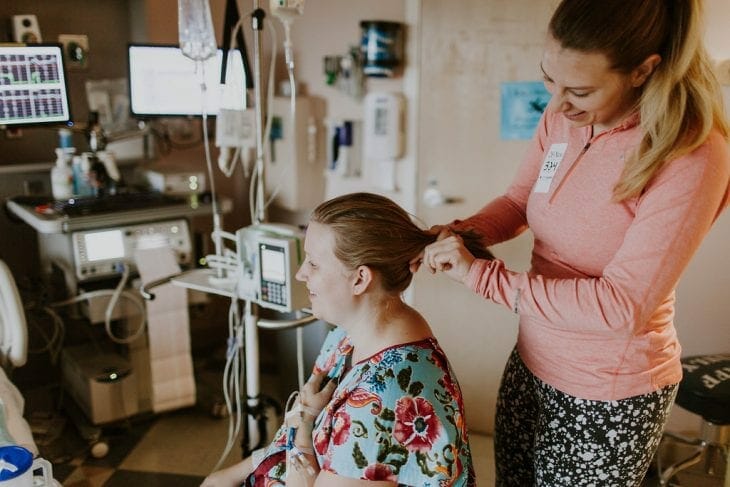
See that IV placed into the side of my wrist though? That was my biggest complaint with being in the hospital! After three attempts to get the IV placed in my arm, they finally had to put it into my wrist meaning I pretty much couldn’t move that hand at all. It also caused my hand to be so swollen I literally couldn’t move my fingers. It was so frustrating but I knew that things like having an IV was just part of having a hospital birth compared to a birth center birth and that it was necessary for them to quickly control my blood pressure if it rose too high.



Through each contraction I would lean on to the bed and they would lose the baby’s heartbeat because of our position. So after trying to get the monitor in the right position for about 10 minutes I finally told my dear nurse that I was okay moving so that they could monitor better.
I was so thankful for the rocking chair in our room and for the next hour I sat there rocking.
It was such a peaceful environment and I just got in serious zen mode during contractions. I felt like I just went to my happy place and would deep breathe through each contraction and then go back to the conversation that was going on.

Contractions were consistent and felt just like they did when I had my first with low back pain so I knew this was it and this is just how I labor.
After I had my first baby I always wondered if it was just a fluke and labor is actually much more difficult then what I experienced. I realized though that apparently my body is just made to have babies.
Every 30 minutes or so Amanda (my nurse) would come in to see how things were going. After only bumping up the Pitocin one time to 4ml they started reducing it by half every 15-30 minutes because the contractions were just one on top of another. That was a really great sign that my body was going through the motions pretty much on their own and the Pitocin was dropped from 4ml to 2ml to 1ml and then to .5ml — which is where it stayed until delivery.
Having the pit at only .5ml was such a great thing! Many people go up to 16-20ml with inductions and so knowing that I didn’t really need the pitocin at that point was really encouraging.
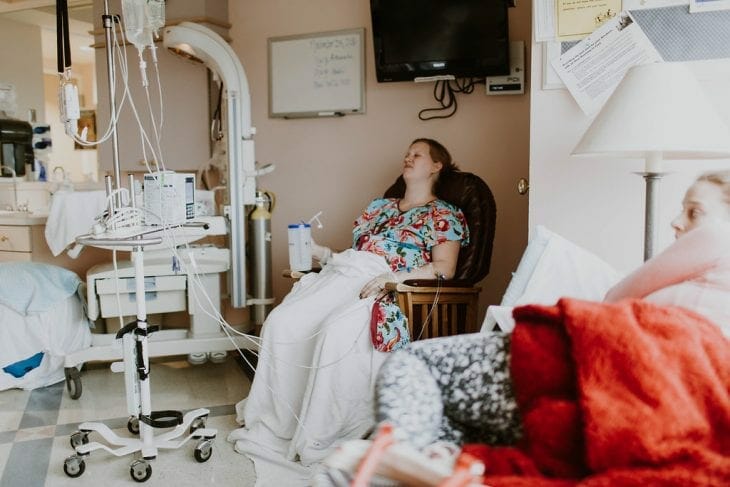
As the intensity picked up though, I started wondering if I would have any energy to push the baby out once the time came and I mentioned asking about pain management options to Justin. I knew he supported me 100% so decided to just ask our nurse what options I had. I knew I definitely did not want an epidural if I could avoid it but I also wasn’t completly opposed to pain meds.
At 2:30, Amanda, my nurse, came in and said she would check me first and then we could talk about pain management options. As I stood up from the rocking chair I felt a little pressure and figured I’d try going to the bathroom before I got in bed to be checked. Of course I couldn’t go to the bathroom but I remember timidly telling Justin I thought there was much more pressure than earlier and I wondered if that’s what they meant what it comes to having to push.
You’d think after already having a baby before I’d have a better idea of what it all felt like. Not true!



Amanda! I love this beautiful story and I can remember all your details too. You are so inspiring to me!! You did an incredible job delivering your sweet girl and I am so thankful to have been there! Hope to see you again some day.. until then I’ll be following your blog! ❤️ your l&d nurse
Wow! Amanda, you are a rockstar! What a whirlwind! Congratulations!! She is beautiful and I just love her name.. <3
The title of this is misleading. I read this expecting an unmedicated induction. That’s not what happened. This was just an epidural-free delivery, which is a totally different title that unmedicated induction.
I couldnt have found your post at a better time. Sitting at 36w5d with slightly too high bp waiting to find out if they are going to induce us or not. I was really hoping for a natural/no intervention labour and delivery, but what is healthiest for mama and baby comes first. Thank you for sharing your wonderful story.
Oh, I’m so glad! Hang in there, momma!! It’s so tough sitting in that unknown just waiting. I’m so grateful for technology though to help doctors make that tough decision of when to call it. Baby will be here snuggled in your arms before you know it!